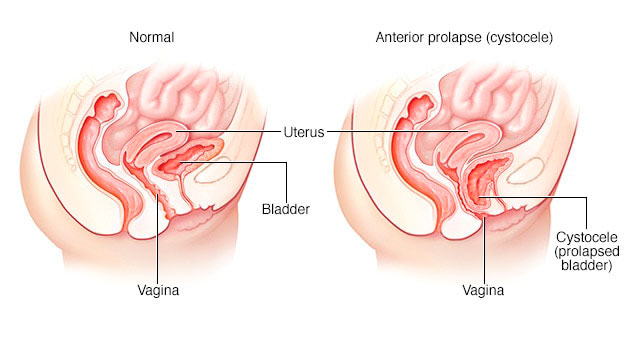
Cystocele
Anterior prolapse, also known as a cystocele (SIS-toe-seel), occurs when the supportive tissue between a woman’s bladder and vaginal wall weakens and stretches, allowing the bladder to bulge into the vagina. Anterior prolapse is also called a prolapsed bladder.
Straining the muscles that support your pelvic organs may lead to anterior prolapse. Such straining occurs during vaginal childbirth or with chronic constipation, violent coughing or heavy lifting. Anterior prolapse also tends to cause problems after menopause, when estrogen levels decrease.
For a mild or moderate anterior prolapse, nonsurgical treatment is often effective. In more severe cases, surgery may be necessary to keep the vagina and other pelvic organs in their proper positions.
Symptoms
In mild cases of anterior prolapse, you may not notice any signs or symptoms. When signs and symptoms occur, they may include:
- A feeling of fullness or pressure in your pelvis and vagina
- Increased discomfort when you strain, cough, bear down or lift
- A feeling that you haven’t completely emptied your bladder after urinating
- Repeated bladder infections
- Pain or urinary leakage during sexual intercourse
- In severe cases, a bulge of tissue that protrudes through your vaginal opening and may feel like sitting on an egg
Signs and symptoms often are especially noticeable after standing for long periods of time and may go away when you lie down.
Causes
Your pelvic floor consists of muscles, ligaments and connective tissues that support your bladder and other pelvic organs. The connections between your pelvic floor muscles and ligaments can weaken over time, as a result of trauma from childbirth or chronic straining of pelvic floor muscles. When this happens, your bladder can slip down lower than normal and bulge into your vagina (anterior prolapse).
Possible causes of anterior prolapse include:
- Pregnancy and vaginal childbirth
- Being overweight or obese
- Repeated heavy lifting
- Straining with bowel movements
- A chronic cough or bronchitis
Risk factors
These factors may increase your risk of anterior prolapse:
- Childbirth. Women who have vaginally delivered one or more children have a higher risk of anterior prolapse.
- Aging. Your risk of anterior prolapse increases as you age. This is especially true after menopause, when your body’s production of estrogen — which helps keep the pelvic floor strong — decreases.
- Hysterectomy. Having your uterus removed may contribute to weakness in your pelvic floor support.
- Genetics. Some women are born with weaker connective tissues, making them more susceptible to anterior prolapse.
- Obesity. Women who are overweight or obese are at higher risk of anterior prolapse.
Prevention
To reduce your risk of developing anterior prolapse, try these self-care measures:
- Perform Kegel exercises on a regular basis. These exercises can strengthen your pelvic floor muscles, and this is especially important after you have a baby.
- Treat and prevent constipation. High-fiber foods can help.
- Avoid heavy lifting, and lift correctly. When lifting, use your legs instead of your waist or back.
- Control coughing. Get treatment for a chronic cough or bronchitis, and don’t smoke.
- Avoid weight gain. Talk to your doctor to determine your ideal weight and get advice on weight-loss strategies, if you need them.
Diagnosis
Diagnosis of anterior prolapse may involve:
- A pelvic exam. You may be examined while lying down and while standing up. During the exam, your doctor looks for a tissue bulge into your vagina that indicates pelvic organ prolapse. You’ll likely be asked to bear down as if during a bowel movement to see how much that affects the degree of prolapse. To check the strength of your pelvic floor muscles, you’ll be asked to contract them, as if you’re trying to stop the stream of urine.
- Filling out a questionnaire. You may fill out a form that helps your doctor assess the degree of your prolapse and how much it affects your quality of life. Information gathered also helps guide treatment decisions.
- Bladder and urine tests. If you have significant prolapse, you might be tested to see how well and completely your bladder empties. Your doctor might also run a test on a urine sample to look for signs of a bladder infection, if it seems that you’re retaining more urine in your bladder than is normal after urinating.
Treatment
Treatment depends on how severe your anterior prolapse is and whether you have any related conditions, such as a uterus that slips into the vaginal canal (uterine prolapse).
Mild cases — those with few or no obvious symptoms — typically don’t require treatment. You could opt for a wait-and-see approach, with occasional visits to your doctor to see if your prolapse is worsening, along with self-care measures, such as exercises that strengthen your pelvic floor muscles.
If self-care measures aren’t effective, anterior prolapse treatment might involve:
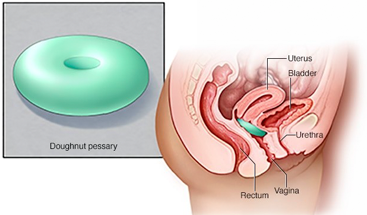
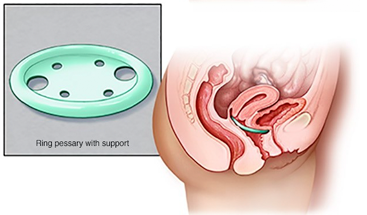
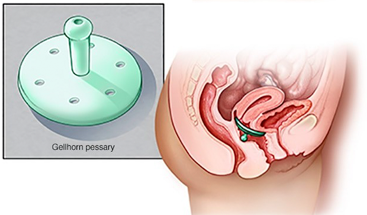
- A supportive device (pessary). A vaginal pessary is a plastic or rubber ring inserted into your vagina to support the bladder. Your doctor or other care provider fits you for the device and shows you how to clean and reinsert it on your own. Many women use pessaries as a temporary alternative to surgery, and some use them when surgery is too risky.
- Estrogen therapy. Your doctor may recommend using estrogen — usually a vaginal cream, pill or ring — especially if you’ve already experienced menopause. This is because estrogen, which helps keep pelvic muscles strong, decreases after menopause.
When surgery is necessary
If you have noticeable, uncomfortable symptoms, anterior prolapse may require surgery.
- How it’s done. Often, the surgery is performed vaginally and involves lifting the prolapsed bladder back into place, removing extra tissue, and tightening the muscles and ligaments of the pelvic floor. Your doctor may use a special type of tissue graft to reinforce vaginal tissues and increase support if your vaginal tissues seem very thin.
- If you have a prolapsed uterus. For anterior prolapse associated with a prolapsed uterus, your doctor may recommend removing the uterus (hysterectomy) in addition to repairing the damaged pelvic floor muscles, ligaments and other tissues.
If you’re thinking about becoming pregnant, your doctor may recommend that you delay surgery until after you’re done having children. Using a pessary may help relieve your symptoms in the meantime. The benefits of surgery can last for many years, but there’s some risk of recurrence — which may mean another surgery at some point.
Dealing with incontinence
If your anterior prolapse is accompanied by stress incontinence — involuntary loss of urine during strenuous activity — your doctor may recommend one of a number of procedures to support the urethra (urethral suspension) and ease your incontinence symptoms.
Lifestyle and home remedies
Kegel exercises strengthen your pelvic floor muscles, which support the uterus, bladder and bowel. A strengthened pelvic floor provides better support for your pelvic organs and relief from symptoms associated with anterior prolapse.
To perform Kegel exercises, follow these steps:
- Tighten (contract) your pelvic floor muscles — the muscles you use to stop urinating.
- Hold the contraction for five seconds, then relax for five seconds. (If this is too difficult, start by holding for two seconds and relaxing for three seconds.).
- Work up to holding the contraction for 10 seconds at a time.
- Do three sets of 10 repetitions of the exercises each day.
Ask your health care provider for feedback on whether you’re using the right muscles. Kegel exercises may be most successful when they’re taught by a physical therapist and reinforced with biofeedback. Biofeedback involves using monitoring devices that help ensure you’re tightening the proper muscles with optimal intensity and length of time.
Once you’ve learned the proper method, you can do Kegel exercises discreetly just about anytime, whether you’re sitting at your desk or relaxing on the couch.

