Rectal prolapse
There are several ways to perform a rectal prolapse surgery. The surgeon will recommend the right method for you, depending on the condition and your general health.
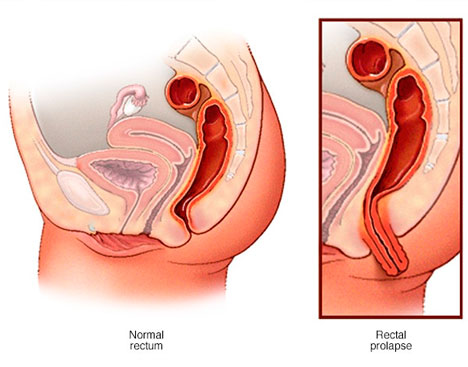
Why is it done?
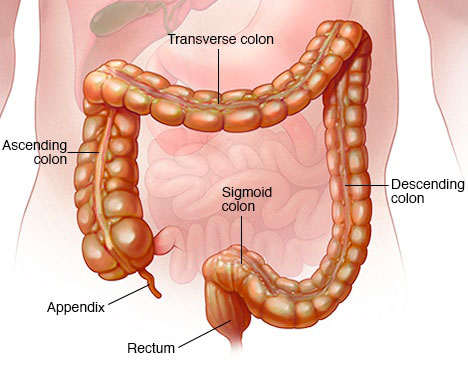
Risks
- Bleeding
- Intestinal obstruction
- Damage to nearby structures, such as nerves and organs
- Narrowing (constriction) of the anal opening
- Infection
- Fistula, an abnormal connection between two parts of the body, such as the rectum and vagina
- Recurrence of rectal prolapse
- Appearance of constipation or worsening
During rectal prolapse surgery
The surgery can be done under general anesthesia, in which case you will be asleep; a spinal block, in which case the lower half of the body falls asleep; or a combination of relaxing medications and local anesthesia to sleep the anus (perianal block).
The approach that your surgeon chooses will depend on several factors, such as your age, other health problems you have, the experience and preferences of the surgeon, and the equipment available. No procedure is considered to be the best of all. Analyze the options with your surgeon.
Types of rectal prolapse surgery:
- Repair of rectal prolapse from the abdomen. Through an incision in the abdomen, the surgeon pulls the rectum to put it back in place. With sutures or a mesh sling, attach the rectum to the posterior wall of the pelvis (sacrum). In some cases, such as when there is a long history of constipation, the surgeon may also remove part of the colon.
- Laparoscopic rectal prolapse surgery. In this procedure, which is also done through the abdomen, several smaller incisions are used. The surgeon inserts special surgical instruments and a tiny camera through the abdominal incisions to repair the rectal prolapse. In an emerging robotic approach, a robot is used to perform the operation.
- Repair of rectal prolapse through the region surrounding the anus (perineal rectosigmoidoscopy). During the most frequent form of this procedure (Altemeier procedure), the surgeon pulls the rectum through the anus, removes part of the rectum and sigmoid, and attaches the remaining part of the rectum to the large intestine (colon). In general, this repair is reserved for people who are not candidates for open or laparoscopic repair. Another method to repair rectal prolapse from the perineum (Delorme’s procedure) is most commonly performed for short prolapses. The lining of the rectum is removed and the muscle layer is folded to shorten the rectum.
If you have rectal prolapse and some other specific disease, such as vaginal prolapse or prolapse of the pelvic organs, you can undergo both repairs in a single surgery.
After rectal prolapse surgery
The doctor is likely to recommend drinking plenty of fluids, consuming stool softeners and a fiber-rich diet in the weeks after surgery to avoid constipation and excessive tension, which could lead to recurrent rectal prolapse. Most people can resume their daily activities after four to six weeks after surgery.
Some people need physiotherapy to relearn how to use the pelvic floor muscles.
Results
The reappearance of rectal prolapse after surgery occurs in about 2 to 5 percent of people. Apparently, it is a little more frequent in people who underwent perineal surgery than in those who underwent abdominal surgery.

